May both periodontal disease and tooth loss increase the risk of dementia?
May both periodontal disease and tooth loss increase the risk of dementia?
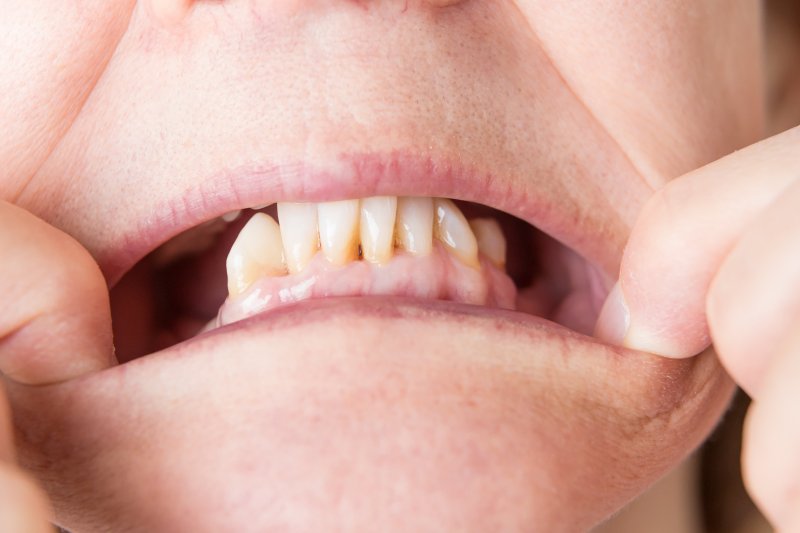
Periodontal disease and missing teeth may seem like problems that only affect your mouth, but did you know that they may be closely related to dementia (Alzheimer's disease)?
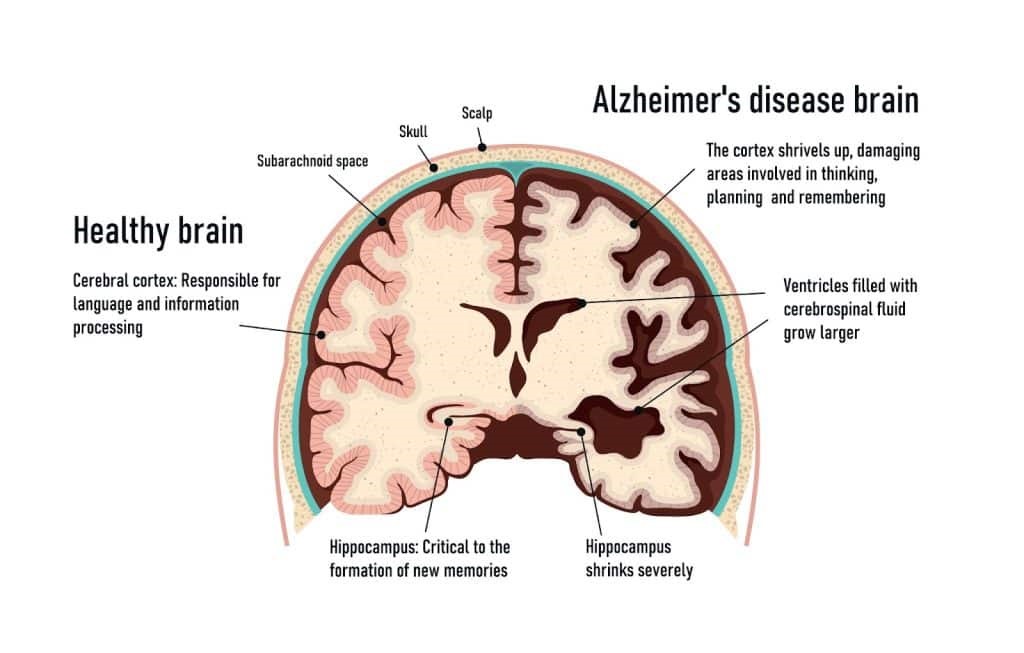
Chronic inflammation and bacterial proliferation caused by periodontal disease may have negative effects on organs throughout the body. Studies have shown that people with periodontal disease have a 10% to 14% higher risk of developing dementia than healthy people; and missing teeth reduce the sensory stimulation of daily chewing to the brain, which may further affect brain function and memory. Japanese scholars found that for elderly people over 60 years old who have less than 20 real teeth, the risk of dementia may increase by 60% to 80%.
These seemingly unrelated issues are actually closely linked. Seeing this data, people have to re-examine the importance of oral health.
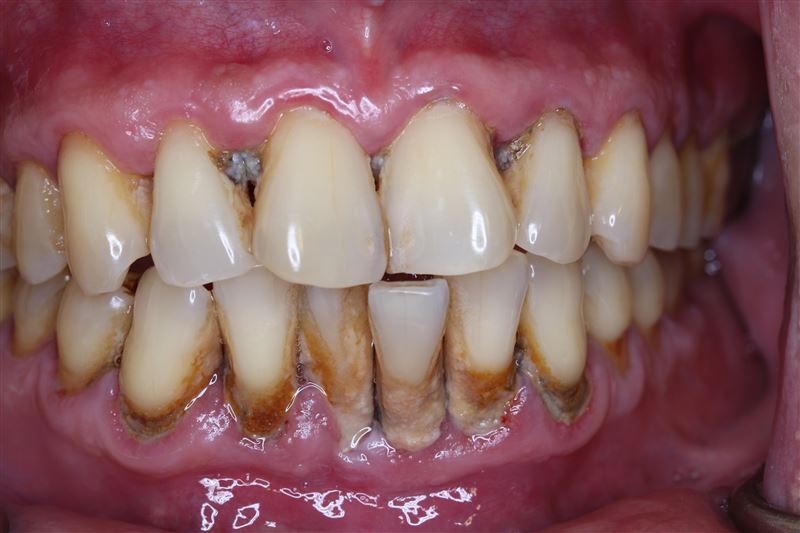
What is the connection between periodontal disease and tooth loss?
There is an inseparable causal relationship between periodontal disease and tooth loss. Periodontal disease is a chronic inflammatory disease caused by bacterial infection that primarily attacks the gums and bone tissue that supports the teeth. As the disease progresses, periodontal disease will gradually destroy the alveolar bone and periodontal ligament, causing the teeth to lose stable support, eventually leading to loose teeth or even falling off.
Initially, periodontal disease may manifest as red and swollen gums, bleeding, bad breath, and then mild gum recession. But if left untreated, the inflammation can progress and affect the bone around the roots of the teeth. When a large amount of alveolar bone is lost, the teeth lose their anchoring foundation, and even healthy teeth may not be able to survive due to insufficient bone mass. This is why periodontal disease is considered one of the main causes of tooth loss in adults.
At the same time, missing teeth may in turn aggravate the progression of periodontal disease. When teeth are missing, adjacent teeth lose support and may tilt or shift, leading to an unbalanced bite that makes it easier for food to accumulate and bacteria to grow. The alveolar bone in the toothless area lacks normal chewing stimulation, which will also accelerate bone atrophy, further weaken the stability of the oral structure, create more space for bacterial invasion, and form a vicious circle.
Therefore, periodontal disease and tooth loss are not independent problems, but a chain reaction that affects each other. Maintaining periodontal health and promptly treating periodontal disease can not only preserve teeth but also help prevent further deterioration of oral function and structure.
What are the systemic health problems caused by periodontal disease?
Periodontal disease is not only an oral problem, but also an invisible threat to overall health. The gums are a structure full of microvessels. Once infected, periodontal disease bacteria will spread throughout the body through the blood circulation, inducing a series of health problems and even making certain chronic diseases more difficult to control. Let’s take a look at the systemic health problems that periodontal disease may cause:
Exacerbation of diabetes
Once periodontal disease bacteria enter the blood, they may interfere with the action of insulin, making blood sugar control more difficult. Studies have shown that if diabetic patients also suffer from periodontal disease, the stability of glycosylated hemoglobin will be affected, further hindering the management of diabetes.
Increased risk of cardiovascular disease
Periodontal disease bacteria not only attack the oral cavity, but may also cause chronic inflammatory reactions in the blood vessel walls, promote the process of arteriosclerosis, and vascular damage can easily increase the risk of myocardial infarction or stroke.
Cognitive Decline and Dementia
In recent years, studies have also found that periodontal disease is closely related to the development of dementia (Alzheimer's disease). People with dementia (Alzheimer's) who also have periodontal disease experience cognitive decline six times faster than those without periodontal disease. Chronic inflammation and bacterial spread caused by periodontal disease may further damage brain health and accelerate the decline of memory and cognitive abilities.
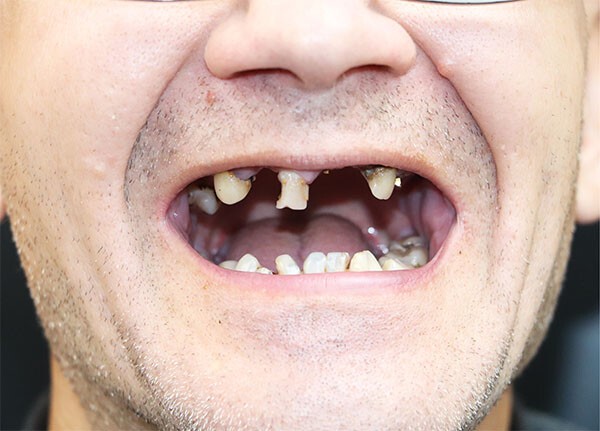
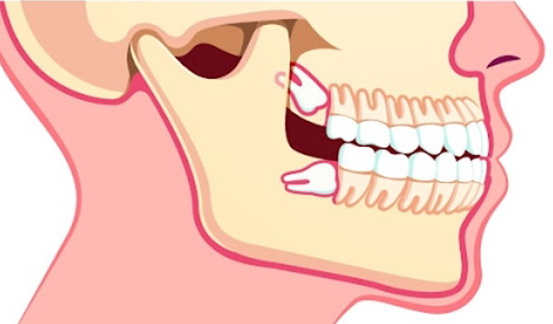
Why does missing teeth affect brain function? Increased risk of dementia?
Missing teeth not only affects eating, but also has potential effects on brain function and even increases the risk of dementia. The chewing function of teeth is not only related to diet, but is also deeply related to maintaining brain health.
The teeth and alveolar bone are tightly connected by a layer of suspensory ligaments called periodontal membrane. When we chew food, the pressure on the tooth roots will compress the microvessels in the periodontal membrane. This physical stimulation can promote blood circulation. The brain plays an active role in maintaining blood circulation in the brain. Not only that, the chewing action also activates brain areas including the hippocampus and gray matter, which are closely related to memory and cognitive function.
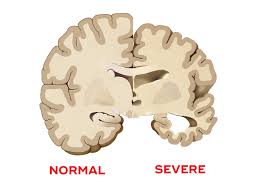
Therefore, lack of sufficient chewing action may reduce stimulation to the brain and further affect brain health. When tooth loss occurs, chewing power will decrease. The more teeth lost, the more serious the loss of chewing function. People with missing teeth are at higher risk of developing dementia, which may be related to reduced chewing function, decreased blood flow to the brain, and reduced neuronal activity.