Beware of Secondary Caries after Dental Filling
Beware of Secondary Caries after Dental Filling
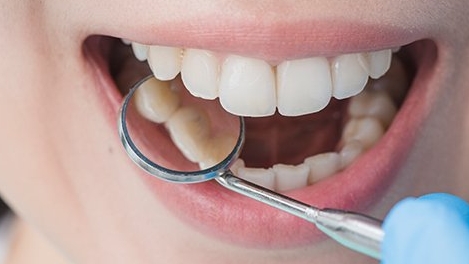
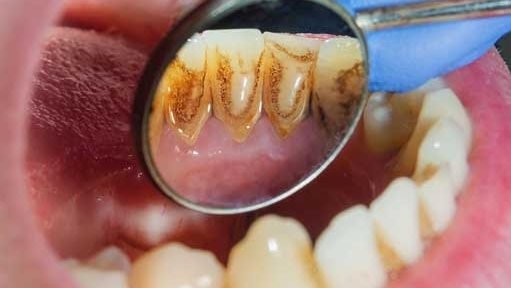
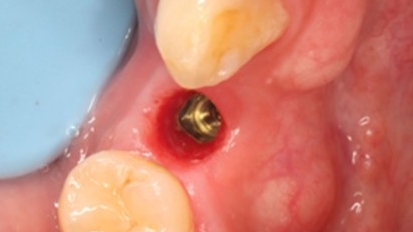
When it comes to tooth decay (dental caries), many people know that damaged teeth can be restored through dental filling. However, some individuals may experience tooth sensitivity, pain, or other discomfort after the filling procedure. Upon medical examination, they are often diagnosed with "secondary caries." As a common complication post-filling, secondary caries acts like an "invisible killer" hiding in the teeth, quietly eroding oral health while frequently going unnoticed.
I. What is Secondary Caries?
Simply put, secondary caries refers to the recurrence of dental caries around or beneath the restoration (filling material) after a tooth has undergone restorative treatment (dental filling). Unlike primary caries, it occurs in concealed locations with subtle early symptoms. Once obvious pain develops, the decay has often damaged the deep dentin or even approached the dental pulp, increasing the complexity of treatment.
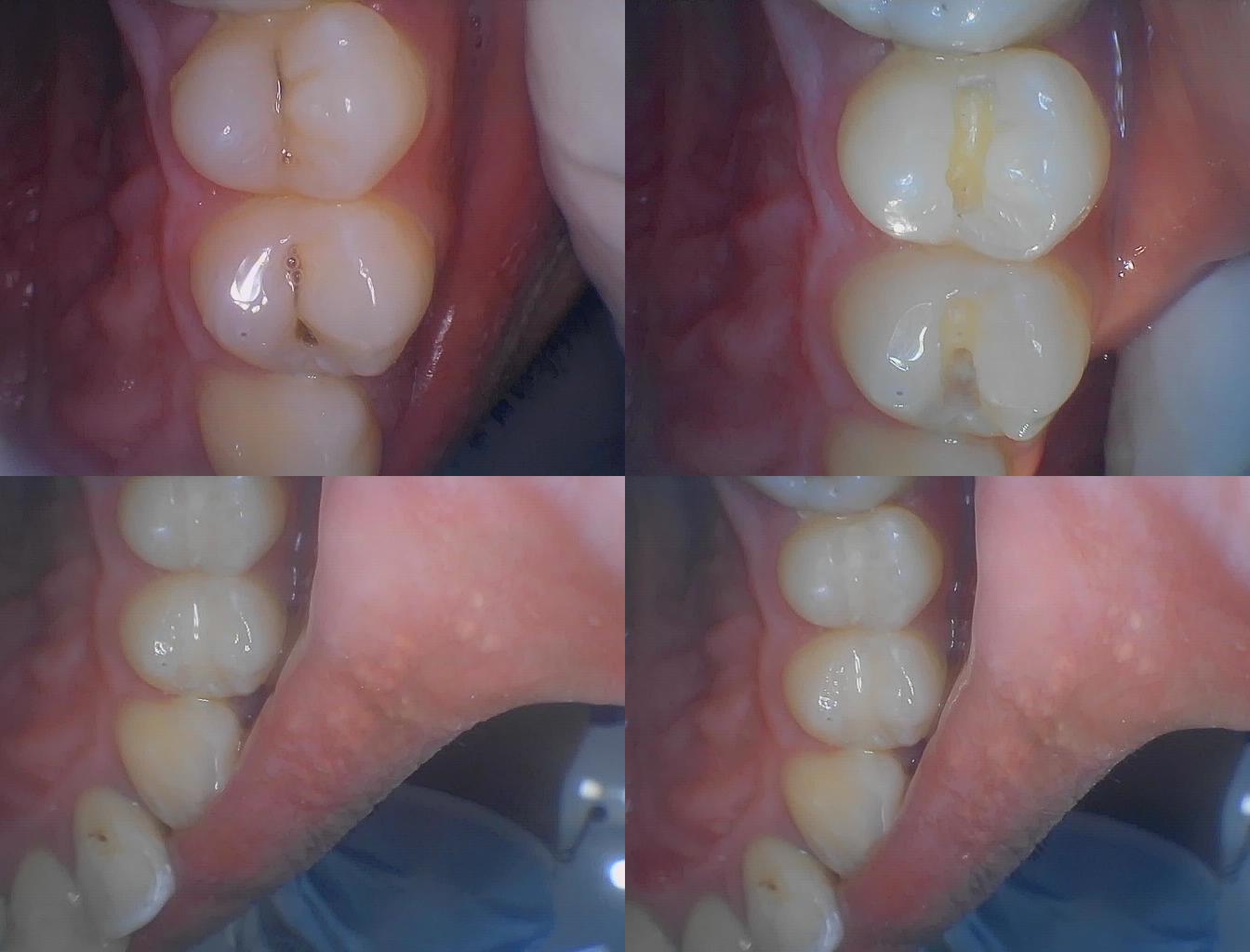
II. Why Does Secondary Caries Recur?
The occurrence of secondary caries is not accidental but results from the combined effect of multiple factors. The core cause lies in the formation of a "hidden pathway" between the tooth and the restoration:
Poor Marginal Adaptation of the Restoration: If the filling material fails to adhere tightly to the tooth's hard tissues during the procedure, tiny gaps form. These gaps are invisible to the naked eye but serve as hiding places for bacteria and food debris, which gradually erode the tooth.
Incomplete Removal of Decayed Tissue Before Filling: If the dentist does not fully eliminate the decayed tissue during the filling process, residual bacteria will continue to multiply, leading to recurrent caries beneath the restoration.
Inadequate Oral Hygiene Maintenance: Failure to maintain proper oral hygiene after filling—such as insufficient brushing or not using dental floss—causes plaque accumulation around the restoration. Long-term plaque irritation triggers secondary caries.
Aging or Damage to Filling Material: Over time, filling materials may wear down or crack. Chewing hard foods can also cause damage, compromising the tooth's protective barrier and allowing bacteria to invade.
Intrinsic Tooth Structure Issues: Certain tooth surfaces, such as fissures and proximal areas, are naturally prone to food and bacteria retention. Even after filling, these areas remain high-risk for secondary caries.
III. Warning Signs of Secondary Caries
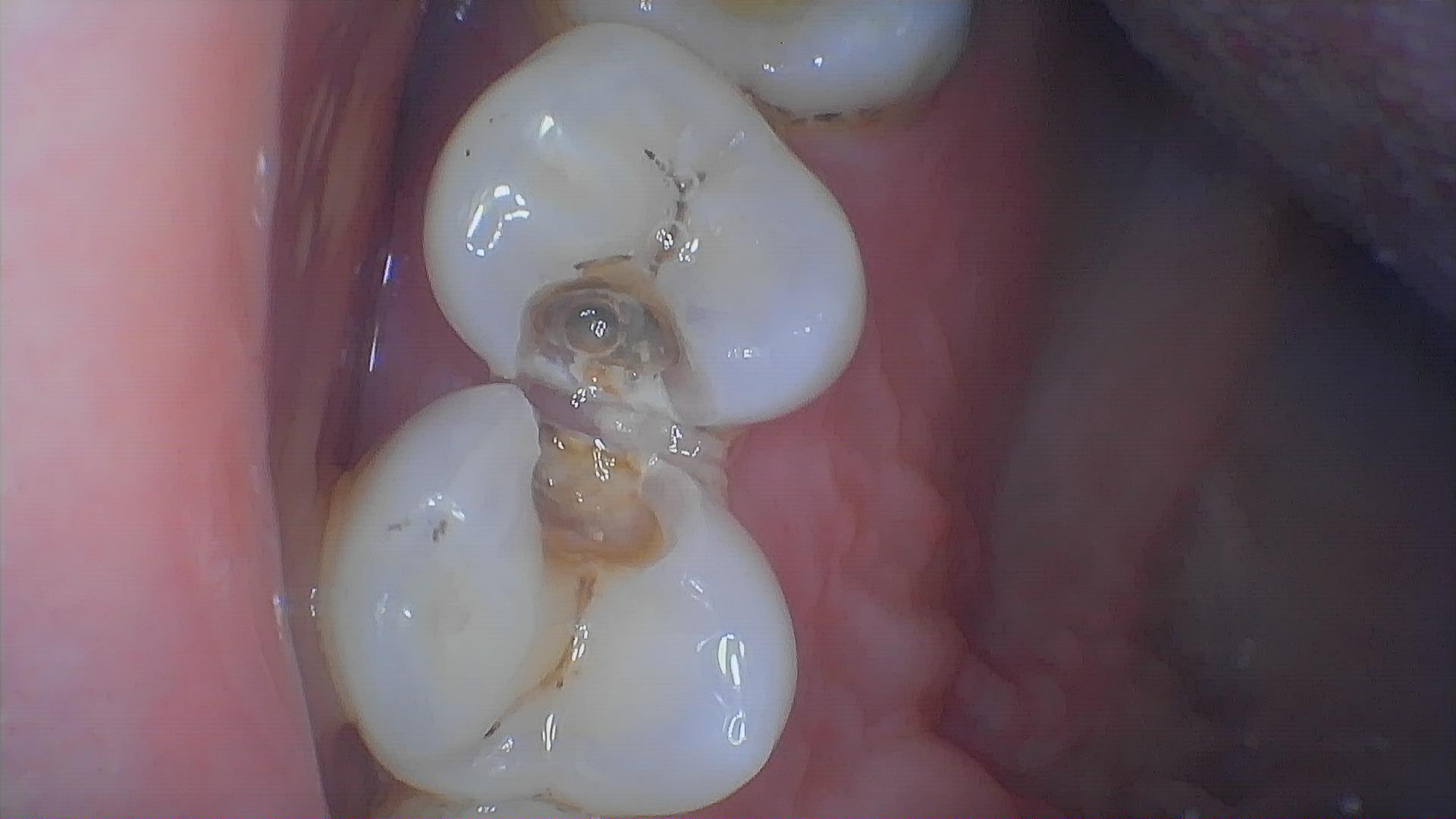
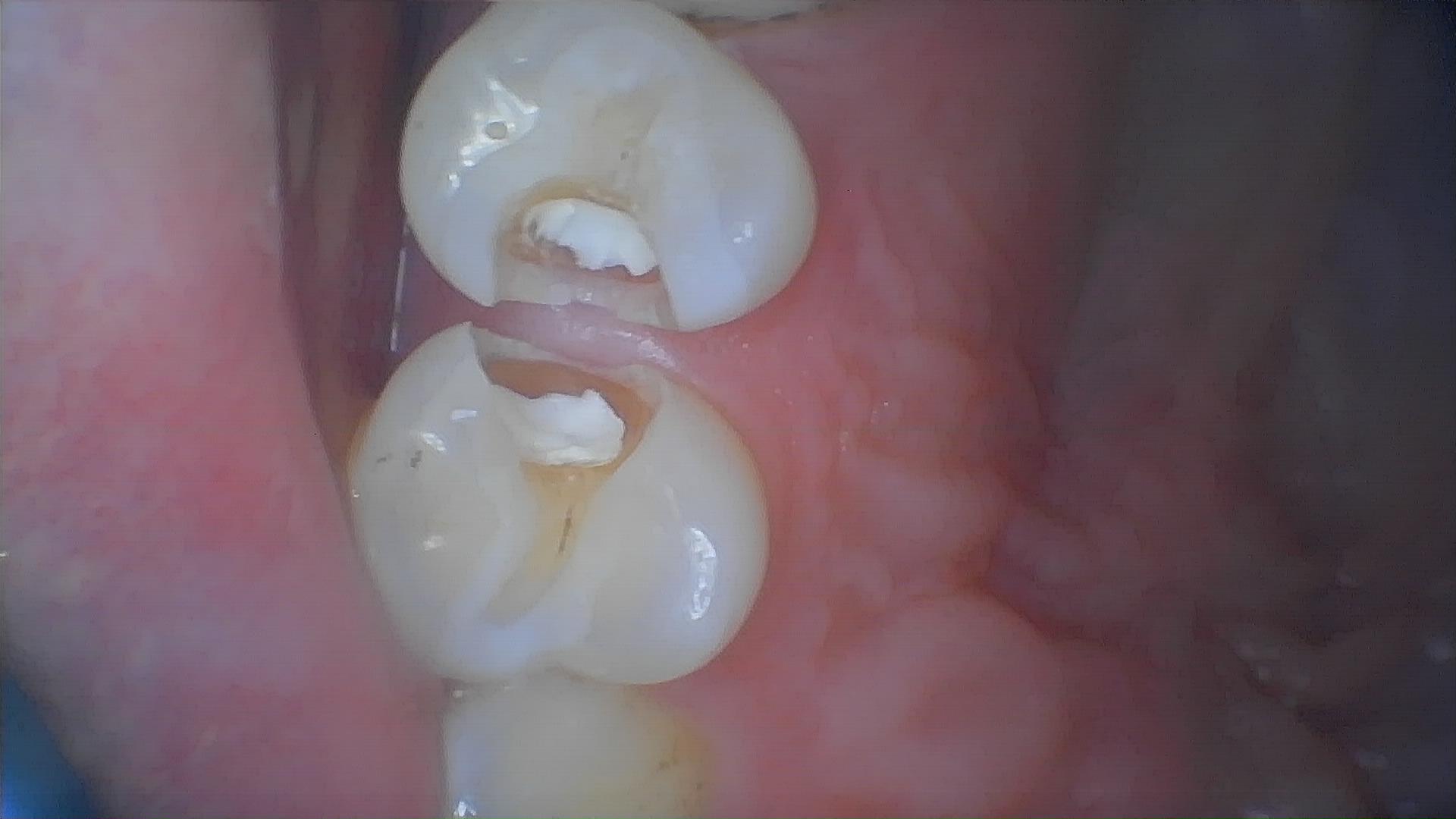
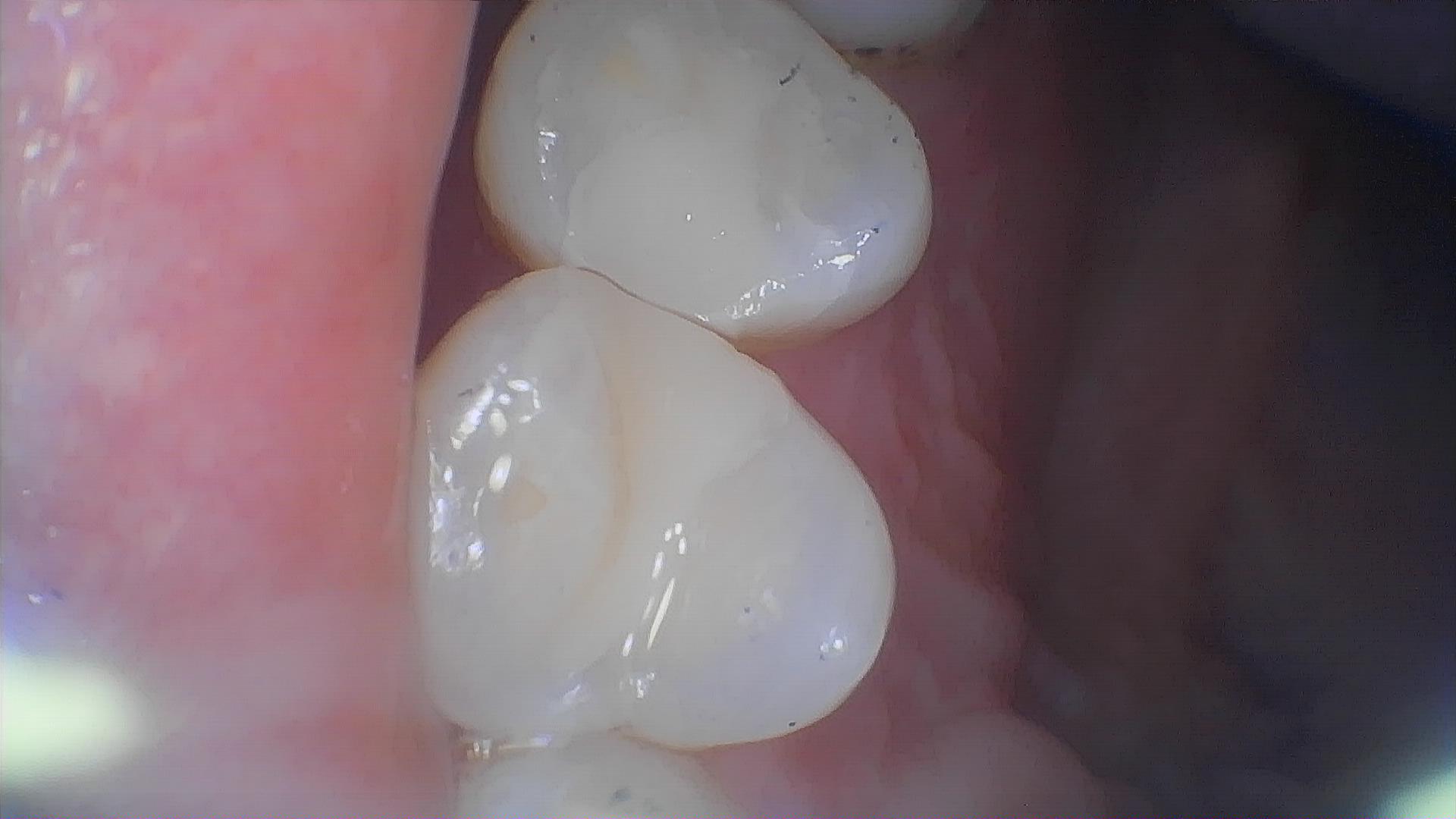
Early symptoms of secondary caries are subtle and easily mistaken for normal post-filling discomfort. However, as the condition progresses, the following typical signs may appear:
Increased tooth sensitivity to cold, heat, acid, or sweet stimuli, manifesting as transient soreness that subsides once the stimulus is removed.
Discoloration (darkening) of the tooth tissue around the restoration, or visible tiny gaps or defects.
Occlusal discomfort or mild pain during eating. In severe cases, the pain may persist and worsen, even leading to pulpitis with symptoms such as spontaneous pain or nocturnal pain.
If any of the above signs occur, seek prompt dental examination to prevent further progression of the condition.
IV. Diagnosis and Treatment of Secondary Caries
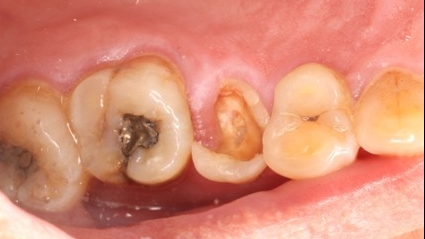
(I) Diagnostic Methods
Dentists primarily diagnose secondary caries through the following approaches:
Visual Inspection and Palpation: Using professional instruments, the dentist observes the restoration margins for discoloration or gaps and uses a probe to check for softened tooth tissue (decayed areas).
Imaging Examinations: Dental X-rays or CBCT (Cone Beam Computed Tomography) can clearly reveal caries-like radiolucencies beneath the restoration, helping determine the depth and extent of decay. This is a crucial basis for diagnosing secondary caries.
(II) Treatment Principles
The core principle of treating secondary caries is "thoroughly removing decay and re-establishing protection":
First, remove the existing restoration and completely eliminate residual decayed tissue to ensure the tooth's hard tissues are healthy.
For shallow caries, after removing the decay, direct re-filling can be performed using materials with better adaptability to the tooth (e.g., resin, glass ionomer cement).
For deep caries that is close to or has damaged the dental pulp, pulp protection treatment (e.g., indirect pulp capping) should be performed first. Once the tooth stabilizes, re-filling is carried out.
If the pulp is already infected (manifesting as pulpitis symptoms), root canal treatment is required to remove the infected pulp tissue. Subsequent protection of the tooth is achieved through filling or crown placement.
V. How to Prevent Secondary Caries?
Secondary caries is not inevitable. The following measures can effectively reduce its incidence:
Choose a Regular Dental Institution and High-Quality Materials: Select a formal dental clinic and an experienced dentist to ensure tight adaptation between the restoration and the tooth. Additionally, choose appropriate filling materials based on the tooth's condition (e.g., resin materials, with high adaptability and wear resistance, are suitable for most locations).
Adhere to Scientific Oral Hygiene Practices: Brush teeth with fluoride toothpaste for at least 2 minutes twice a day, focusing on cleaning around the restoration. Rinse the mouth promptly after meals, and use dental floss or an oral irrigator to clean interproximal gaps to avoid food residue.
Regular Dental Check-Ups: Undergo oral examinations every 6-12 months after filling. Dentists can detect issues such as restoration wear or poor marginal adaptation early and intervene promptly. Receive professional teeth cleaning (scaling) 1-2 times a year to remove tartar and plaque.
Develop Healthy Eating Habits: Reduce intake of sugary and acidic foods, avoid frequent snacking, and lower the risk of tooth erosion. Chew sugar-free gum after meals to stimulate saliva secretion, which neutralizes oral acidity.
Avoid Damaging the Restoration: Refrain from chewing hard foods (e.g., nuts, bones) after filling to prevent restoration damage or dislodgement.