Analysis of the Etiology of Root Canal Calcification from a Dental Professional Perspective
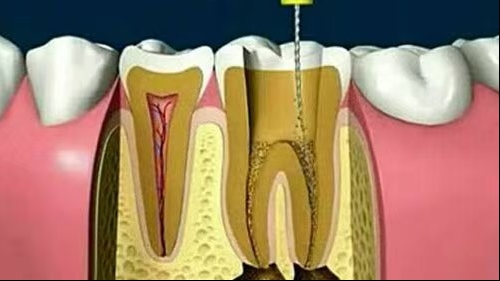
Analysisof the Etiology of Root Canal Calcification from a Dental Professional Perspective Root canal calcification is clinically characterized by canal narrowing, obliteration, and blurred or absent root canal images on radiographs. It is essentially a condition of abnormal dentin mineral deposition, which gradually fills the root canal system. This paper systematically analyzes the causes of root canal calcification from professional perspectives including dental physiology, pathology, irritating factors, age-related changes, and reparative responses.
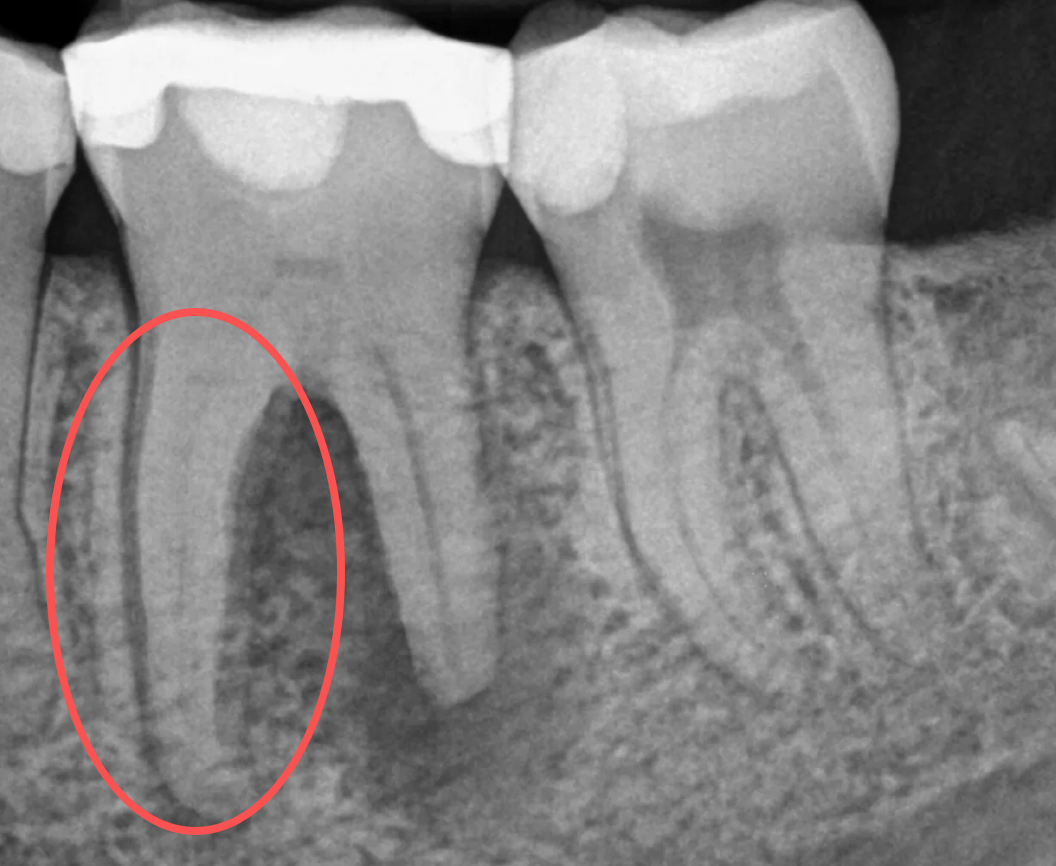
I. Core Mechanism: Excessive Mineralized Repair of Odontoblasts
The root canal wall is formed by the secretion and mineralization of dentin matrix by odontoblasts. Under normal physiological conditions, only primary or secondary dentin is formed. Under persistent stimulation, the production of tertiary dentin (reparative dentin) is induced. When stimulation is repeated and intense, pathological mineral deposition occurs, eventually leading to root canal stenosis or even complete obliteration. In brief:Root canal calcification is an excessive defensive mineralization response of the dental pulp to chronic irritation.
II. Major Etiological Factors
1. Age-Related Physiological Calcification (Most Common) With increasing age, the dental pulp gradually atrophies and fibrosis, and odontoblasts continuously secrete mineralized matrix slowly. Manifested as deposition of secondary dentin, leading to reduced root canal space and narrowing of root canals.Characteristics: mostly bilateral and multi-tooth involvement with slow progression. 2. Chronic Pulpitis (Primary Pathological Factor) Deep caries, cracked teeth, attrition, and periodontal retrograde infection result in chronic pulpitis. Long-term low-grade inflammation stimulates the dental pulp and induces massive formation of reparative dentin.Commonly seen as localized calcification in single teeth, mostly starting from the apical third or coronal portion. 3. Mechanical Trauma and Microtrauma Occlusal trauma Excessive tooth preparation for fixed prosthodontics History of dental trauma (impact, biting hard objects) Mechanical irritation directly damages the odontoblastic layer and triggers a strong reparative response with rapid calcific obliteration. 4. Chemical and Thermal Irritation Irritation from restorative materials (direct restoration without base) Abnormal demineralization and remineralization caused by acid erosion Insufficient water cooling during tooth preparation leading to high temperature All these factors cause chronic dental pulp injury and promote calcification. 5. Periodontally Derived Irritation (Retrograde Root Canal Calcification) Deep periodontal pockets and periodontal-endodontic lesions Chronic periapical inflammation and alveolar bone resorption Irritants penetrate the dental pulp through the apical foramen and lateral canals, inducing calcific obliteration in the apical segment. 6. Systemic Factors (Contributing Factors) Metabolic disorders: hypercalcemia, abnormal parathyroid function Genetic predisposition: inherent tendency of dental hard tissue mineralization in some individuals Systemic medications or diseases affecting pulp blood flow and mineralization regulation Systemic factors mostly serve as aggravating factors rather than independent primary causes.
7. Iatrogenic Factors
Previous inadequate root canal treatment or resinifying therapy
Inadequate base placement and residual caries leading to chronic irritation
Poor marginal adaptation of restorations causing long-term microleakage